Preoperative procedures for patient care are a vital component of the surgical process. They aim to make surgery more effective by considering objective clinical metrics and patient experience and satisfaction.
These preparatory steps are instrumental in assessing the patient’s physical and mental well-being and screening and proactively managing their potential risks. Each element of this process is vital in ensuring that patients are well-prepared for their surgical journey
Some procedures involve the patients, such as shared decisions. Others require a review of the patient’s health history and comorbidities. While others are physical, such as proper surgical marking.
This article overviews various preoperative procedures that help improve surgical success and efficacy.
Patients’ subjective experiences and their perceptions are crucial. Their overall satisfaction with a surgical procedure is one of the essential measures of surgical success.
The shared decision-making and informed consent processes actively involve patients in their preoperative care and allow them to express their preferences. They can ask pertinent questions on accuracy, benefits, risks, and alternatives to planned procedures.
All these factors have been shown to significantly increase patient satisfaction and surgical success by raising patient understanding, improving compliance with treatment regimens, mitigating decision-related conflicts, and reducing potential legal and ethical complications.
Some steps that can be taken to improve patient satisfaction regarding the shared decision-making and informed consent process include:
- Starting this process at the earliest preoperative point involves the patient and all members of a multidisciplinary surgical team that will take an active role in their care.
- Exchanging information relevant to the individual patient, including general and specific risks, specific aspects of their perioperative pathway, modifiable risks, and psychological readiness.
- Encouraging patients to express what is important to them and ask any questions they may have.
- Allowing people close to them to be a part of the shared decision-making process.
- Including the shared decision-making consultation in the patient’s medical notes, allowing easy access to anyone in the future.
2. Patient self-screening health questionnaire
Patient self-screening health questionnaires play a pivotal role in improving surgical outcomes by providing a standardized, often electronic, assessment tool that patients complete at the outset of their surgical journey. These questionnaires capture vital information about a patient’s medical, surgical, and social history.

By collecting this information early in the process, healthcare providers gain valuable insights that can be used to proactively identify potential health risks and optimize management strategies. This results in better surgical outcomes, reduced complications, and better patient experiences.
A key benefit of these self-screening questionnaires is risk stratification. Through the data collected, healthcare teams can categorize patients into different risk levels, with high-risk patients identified promptly. This early identification enables healthcare providers to plan appropriate interventions to mitigate potential risks, whether it involves intensive preoperative preparation or adjusting planned surgical techniques.
However, low-risk patients can get streamlined care, including remote consultations, making more efficient use of healthcare resources.
Fostering effective patient-provider communication is another significant advantage of these questionnaires, as patients are encouraged to be more proactive in sharing their health information, concerns, and expectations. This leads to a stronger patient-provider relationship and a clearer understanding of the patient’s needs. This has been shown to improve patient satisfaction and surgical outcomes further.
Lastly, these questionnaires facilitate efficient resource allocation. Patients at lower risk can be managed remotely, freeing up in-person resources for those at higher risk. This optimizes resource utilization and prevents overburdening the healthcare system, a factor which has improved the safety and success of medical and surgical care.
3. Proper surgical marking
The preoperative marking process refers to visually identifying and marking the intended surgical site on a patient’s body before a surgical procedure. This ensures the planned procedure is performed on the right side, part, and body level. This critical process in surgical preparation ensures accuracy, safety, and precision during the operation, which improves surgical outcomes.
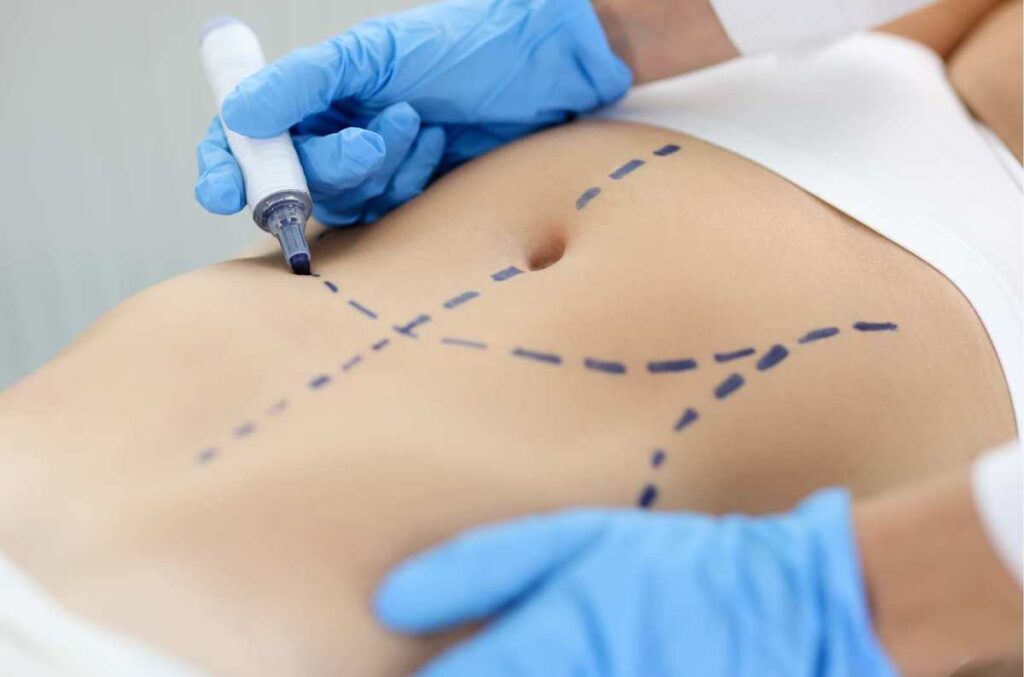
The practice of proper preoperative surgical marking can help improve surgical success in several ways:
- Allows surgeons a clear roadmap during the operation, improving surgical accuracy and reducing errors.
- Improves communication and teamwork within the surgical team, minimizing confusion and errors during the procedure.
- Provides visual confirmation for the patient, which provides reassurance, fosters trust, and reduces anxiety before the operation.
The Universal Protocol and WHO Safer Surgery Checklist provide comprehensive preoperative surgical site marking recommendations. These guidelines are designed to standardize the process and improve surgical outcomes. Key recommendations include:
- Marking for procedures with right/left distinction or multiple structures
- Using clear and unambiguous markings
- Ensuring visibility after draping
- Using smudge-resistant ink
- Avoiding sole reliance on adhesive markers
- Maintaining consistent protocols
- Involving patients in the marking process to prevent errors
4. Screening for patient comorbidities
Screening for patient comorbidities is integral to improving surgical success by addressing the additional health conditions that can significantly impact surgical outcomes.
The presence of comorbid diseases in patients, such as diabetes, uncontrolled hypertension, coronary artery disease, pulmonary, renal, and liver impairments, or even mental health issues, can pose a considerable risk to the success of surgical procedures. Early identification, documentation, and appropriate management of these conditions by the medical team are essential in improving surgical outcomes.
Uncontrolled or poorly managed comorbidities should be addressed before the planned surgical procedure. This proactive approach by a multidisciplinary team minimizes potential health complications and unforeseen risks, contributing to a higher likelihood of surgical success.
5. Evaluating functional capacity and physical fitness
The assessment of functional capacity and physical fitness evaluates the patient’s ability to perform activities of daily living that require sustained aerobic metabolism. This assessment allows the surgical team to see how a patient would perform under physiological stress such as surgery.
Poor functional capacity and physical fitness have been shown to negatively affect surgical success by increasing post-operative complication rates, having poorer long-term health outcomes, and increasing the risk of death.
Suppose patients are found to have poor functional or exercise capacity during this evaluation. In that case, specific steps can be taken preoperatively to improve their status and, therefore, the likelihood of surgical success.
Based on their baseline functional capacity, patients may be recommended to do general exercises, focused exercises for those at moderate risk, or specialized low-intensity workouts designed for high-risk patients. Very unfit patients should be counseled to gradually improve their physical tolerance and set realistic short-term fitness goals.
Example functional capacity and physical fitness evaluation format and suggested interventions:
| Evaluating exercise intensity | Low intensity | Moderate intensity | Vigorous intensity |
| Borg Rating of Perceived Exertion (RPE)* | 0–3 Rest-moderate | 5–7 Somewhat hard-hard | 8–10 Very hard-maximal |
| Talk test | Easy to breathe and carry on a conversation | Breathing more heavily, can only complete a couple of sentences | Breathing very hard, can only say a few words |
| Heart rate range** | <55% of maximum heart rate | 55–75% of maximum heart rate | >75% of maximum heart rate |
| Examples of suggested exercises | Slow walk | Brisk walk, cycling <10 miles/hr, general gardening, dancing | Aerobic dancing, running, cycling >10 miles/hr., soccer, heavy gardening, climbing stairs, swimming laps |
*This scale of measures how hard you feel like your body is working.
**The estimated maximum heart rate is calculated using the following formula HR = 220 – age

