Key points
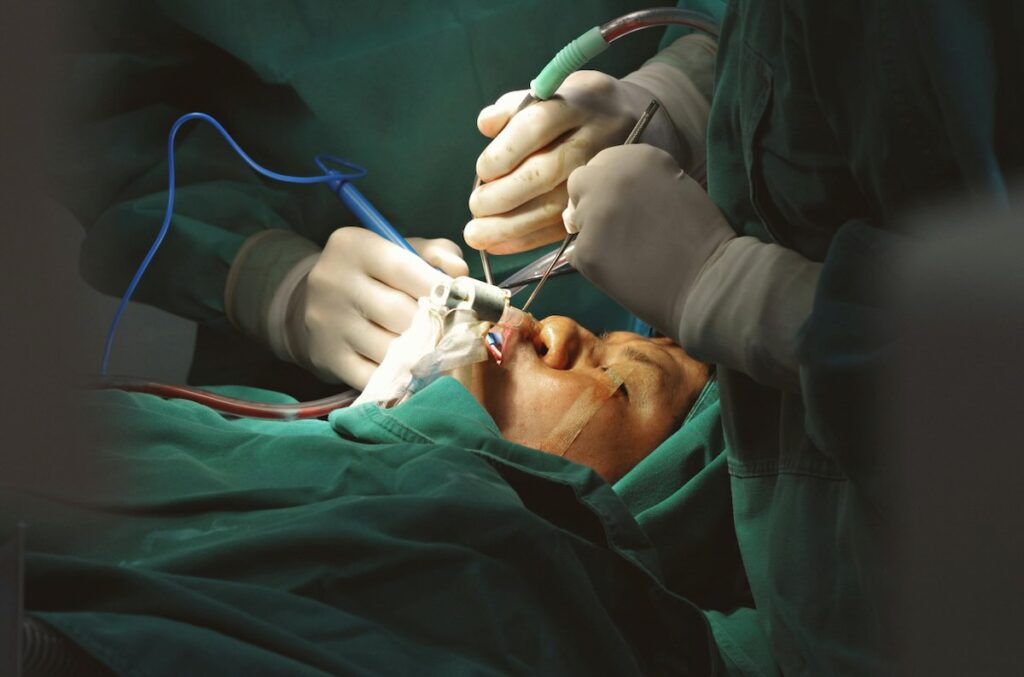
- Cosmetic breast and body contouring procedures demand millimeter-level precision that depends on direct visualization of the surgical cavity.
- Fiber optic retractors pose documented burn risks; cordless LED systems eliminate thermal hazards while matching surgical light standards.
- Distributors sourcing for plastic surgeons should evaluate illumination output, thermal safety, ergonomics, and total cost of ownership.
Plastic surgery and cosmetic surgery relies on millimeter-level precision. A breast augmentation pocket dissected too far inferiorly creates a visible double-bubble deformity. A liposuction cannula that strays into the wrong tissue plane causes contour irregularities that persist for years. Visualization determines results in procedures where outcomes are measured in symmetry and smooth contours.
The numbers reflect sustained demand for these procedures. According to the American Society of Plastic Surgeons statistics, liposuction remained the top cosmetic surgery, followed by breast augmentation, tummy tucks, and breast lifts. Body contouring procedures grew further in 2024, driven partly by patients addressing skin laxity after weight loss from GLP-1 medications.
However, the surgical lighting used in many operating rooms was designed for open abdominal or cardiac procedures, not the deep pockets and narrow incisions typical of cosmetic surgery.
This article examines the specific visualization challenges in breast and body contouring procedures, compares available lighting technologies, and outlines what distributors should evaluate when sourcing illumination solutions for plastic surgeons. Innovative solutions like the Yasui koplight™ literally shed light in this area.
Contents
Why does visualization matter in cosmetic breast surgery?
Breast augmentation through the inframammary approach remains the most common technique precisely because it offers direct visualization of the breast pocket. The surgeon can see the boundaries of the dissection, identify bleeding vessels, and control the implant position with precision. Studies comparing surgical approaches consistently cite visualization as the deciding factor in approach selection.
The transaxillary approach illustrates what happens when visualization is compromised. A study in Plastic and Reconstructive Surgery described the approach’s “main disadvantage” as “the lack of visualization of the implant pocket, necessitating blind, blunt dissection of the pectoral muscle origins.” Blind dissection increases the risk of implant malposition, asymmetry, and the need for revision surgery. The same study noted that endoscopic assistance was developed specifically to address this visualization deficit.

Pocket dissection demands precise control of anatomical boundaries. In subpectoral placement, the surgeon must release the pectoralis major origin while preserving the inframammary fold fascial attachments. A retrospective study of 251 patients found that meticulous dissection under direct endoscopic vision could avoid destruction of fascial structures that prevent implant malposition. The study reported a 0.4% rate of bottoming-out deformity with this visualization approach.
Breast reconstruction after mastectomy presents additional visualization challenges, as detailed in our overview of modern breast surgery devices. Skin-sparing and nipple-sparing mastectomies leave thin skin flaps that are vulnerable to necrosis if perfusion is compromised, with incidence of mastectomy skin flap necrosis ranging from 5% to 30% in the literature. Clear visualization of tissue color, bleeding patterns, and flap thickness during the procedure helps surgeons assess viability and make intraoperative decisions about tissue preservation.
What are the visualization challenges in body contouring?
Abdominoplasty involves dissection through multiple tissue layers across a wide operative field. The surgeon must visualize Scarpa’s fascia, identify perforating vessels, and assess skin flap viability across the entire abdominal expanse. Techniques described in Annals of Plastic Surgery emphasize the need for clear visualization during ultrasound-assisted liposuction of the abdominal flap, where the surgeon marks the future supraumbilical midline and semilunaris lines for muscle definition.
Liposuction adds another dimension of visualization difficulty. The cannula moves through subcutaneous tissue tunnels that are inherently narrow and deep. The surgeon must maintain awareness of the cannula tip position to avoid penetrating into unsafe planes or creating contour irregularities. Modern 360-degree liposuction techniques, which address the abdomen, flanks, and lower back simultaneously, require the surgeon to maintain spatial orientation while working through multiple small incisions.
The fleur-de-lis abdominoplasty, used frequently in post-bariatric patients, combines vertical and horizontal tissue excision. A description in a recent peer-reviewed chapter notes that “careful attention is directed toward identifying potential abdominal hernias that may require repair” during this dissection, since missed hernias become postoperative complications. The extended operative field in these cases makes consistent illumination across all working areas particularly challenging.
Skin flap viability assessment has become increasingly sophisticated with technologies like indocyanine green (ICG) angiography, which visualizes perfusion in real time. These adjunct technologies demonstrate that surgeons recognize the limitations of relying on clinical judgment alone for tissue assessment. The meta-analyses showing reduced necrosis rates with perfusion imaging underscore how much visualization quality affects outcomes.
How do overhead surgical lights fall short in cosmetic procedures?
Geometry is surgical lights’ fundamental limitation. Light travels in straight lines, and the surgeon’s body, hands, and instruments inevitably obstruct the path between an overhead source and a deep operative cavity. Research published in The Surgery Journal found that surgeons adjust overhead lights every 7.5 minutes on average, and in 97% of cases, the surgeon pauses the procedure to make the adjustment.
The same study cited a qualitative survey of 12 breast surgeons in which 92% did not prefer headlights during surgery. Their reasons included insufficient light for deep cavities, persistent shadows and glare, head and neck strain from the headlight weight, constant adjustment requirements, and contamination concerns. These findings suggest that neither overhead lights nor headlights adequately address the visualization needs of breast surgery.
The challenges compound in procedures involving multiple incision sites or extended operative fields. A liposuction case treating the abdomen, flanks, and back requires repositioning the patient and the lighting multiple times. Each transition introduces potential for contamination of sterile light handles; one study found that 50% of randomly selected sterile light handles in hip replacement surgery harbored bacterial cultures.
For cosmetic procedures where aesthetic outcomes define success, these lighting limitations translate directly to results. A surgeon who cannot clearly visualize the tissue being dissected must rely on tactile feedback alone, which introduces variability. The push toward smaller incisions and minimally invasive techniques in cosmetic surgery, driven by patient demand for reduced scarring, further constrains the available light path from overhead sources.
What lighting solutions exist for plastic surgeons?
Surgeons have three main options for supplementing overhead illumination: headlights, fiber optic lighted retractors, and LED lighted retractors. Each addresses the fundamental problem of delivering light into the operative cavity, but with different trade-offs in safety, convenience, and illumination quality.
Headlights attach to the surgeon’s head and direct light along the surgeon’s line of sight. They eliminate the shadow cast by the surgeon’s body, since the light source moves with the surgeon’s gaze. The drawbacks, as documented in the breast surgeon survey, include the physical weight causing neck strain over long procedures, the need for constant head positioning to maintain illumination, and the tethering cable that restricts movement. Studies have linked frequent headlight use to cervical degenerative disc disease in surgeons.
Fiber optic lighted retractors combine tissue retraction with illumination in a single instrument. The Tebbetts and Ferriera retractors are widely used in breast surgery for this purpose. Light from an external halogen or xenon source travels through a fiber optic cable to the retractor blade, illuminating the tissue being retracted. These systems require a dedicated light source unit, cable connections, and careful management of the cable during the procedure. There are better options.
LED lighted retractors represent the newest category. These cordless instruments contain battery-powered LED light sources within the retractor handle, eliminating cables and external light sources. The koplight™ from Yasui exemplifies this design, using a transparent polycarbonate blade that transmits light from the handle-mounted LED directly into the surgical cavity. The cordless design removes the cable management issues inherent in fiber optic systems.
The choice of lighting technology affects both workflow and safety for plastic surgeons who use retractors routinely in breast surgery.
LED vs. fiber optic: which is safer for cosmetic surgery?
The safety comparison between LED and fiber optic illumination centers on thermal risk. Fiber optic cables transmit light from high-intensity halogen or xenon sources, and this light energy converts to heat at the cable termination point. One study found that fiber optic cable tips can reach 225°C within 15 seconds and 239°C (462°F) in under 10 minutes. Contact with these surfaces causes skin burns almost immediately.
The FDA’s adverse event database has logged more than 30 cases of patients sustaining burns during breast surgery from heat generated at the connection between optical cables and lighted retractors. In 2012, the manufacturer of Snowden-Pencer Tebbetts lighted retractors issued an urgent safety notice advising against using optical cables larger than 3.5 mm due to thermal injury risk. Despite this warning, burns have continued to occur.

The injury mechanism relates to the size mismatch between the optical cable and the retractor connector. Light energy is lost as heat at the junction when the cable caliber exceeds the connector diameter. A comparative study measured temperatures generated by different cable sizes and found that larger cables produced temperatures sufficient to cause partial-thickness burns within seconds of contact.
LED light sources operate on fundamentally different physics. LEDs convert electrical energy to light with high efficiency and minimal heat generation. The operating temperatures of LED-based retractors remain well below thresholds that could damage tissue. This eliminates the burn risk that has prompted FDA safety alerts for fiber optic systems.
Beyond thermal safety, the cordless design of LED retractors removes cable-related hazards from the surgical field. Fiber optic cables create trip hazards, can become entangled with other instruments, and require careful routing to prevent kinking that degrades illumination. Our Ferreira and Tebbetts retractor alternatives article discusses these practical limitations in detail.
What should distributors look for when sourcing illuminated retractors?
Medical device distributors serving plastic surgeons should evaluate illuminated retractors across several dimensions: illumination specifications, safety profile, ergonomics, sterilization requirements, and total cost of ownership.
Illumination output should match the requirements specified in IEC 60601-2-41, the international standard for surgical luminaires. This standard calls for central illuminance of 40,000–160,000 lux at 1 meter working distance, with color rendering index (CRI) of 85 or higher. Products that meet these specifications provide illumination comparable to overhead surgical lights while delivering that light directly into the operative cavity.
The safety profile encompasses thermal risk, electrical safety, and material biocompatibility. LED-based systems eliminate the thermal hazards associated with fiber optic cables. Non-conductive blade materials reduce the risk of electrical arcing when electrosurgical instruments contact the retractor, a consideration that has prompted the development of plastic surgical retractors as alternatives to metal.
Ergonomic factors affect surgeon adoption and sustained use. Weight matters for handheld instruments used throughout multi-hour procedures. The koplight™ weighs 100–150 grams including batteries, compared with metal retractors that weigh substantially more. Cordless operation eliminates the cable management that interrupts workflow with fiber optic systems.
Sterilization requirements affect per-procedure costs and infection risk. Systems with disposable blade components and reusable handles offer a middle path between fully disposable instruments and fully reusable systems that require complete reprocessing. Single-use blades eliminate cross-contamination risk while reusable LED handles reduce per-case costs compared with fully disposable options.
Total cost of ownership extends beyond acquisition price. Fiber optic systems require light source units (US$5,000-$20,000 for halogen), cables (US$300-$1,300), sterilization trays, and ongoing maintenance. Cordless LED systems require blade inventory and battery replacement. Distributors should help their surgical customers model these ongoing costs when evaluating options.
Illumination to meet cosmetic surgery’s demands
Cosmetic plastic surgery has evolved toward smaller incisions, more precise dissection, and faster patient recovery. These advances increase the demands on surgical visualization. The deep pockets of breast augmentation, the extended operative fields of abdominoplasty, and the subcutaneous tunnels of liposuction all require illumination that overhead surgical lights cannot reliably deliver.
LED lighted retractors address these visualization challenges while eliminating the thermal hazards that have prompted FDA safety notices for fiber optic systems. The combination of direct in-cavity illumination, cordless operation, and thermal safety makes these instruments well-suited to the specific requirements of cosmetic breast and body contouring procedures.

Dr. Tomoyuki Yano, FACS, Department Director of Plastic and Reconstructive Surgery at the Cancer Institute Hospital of JFCR in Japan, said, “I use the koplight™ in breast reconstruction and in many other major surgeries. It’s lightweight and easy to use. Since it has no cord, the koplight™ provides an outstanding level of convenience.”
Add the koplight™ to your cosmetic surgery portfolio
The koplight™ cordless lighted retractor delivers 40,000+ lux illumination through a transparent polycarbonate blade, providing the direct in-cavity lighting that cosmetic breast and body contouring procedures demand. The LED-based design eliminates thermal risks associated with fiber optic systems while reducing setup time and cable management.
Eight blade sizes accommodate procedures from breast augmentation pocket dissection to abdominoplasty flap elevation. The system is FDA-registered and carries EU MDR certification. Contact us at Yasui for distributor pricing and product samples.