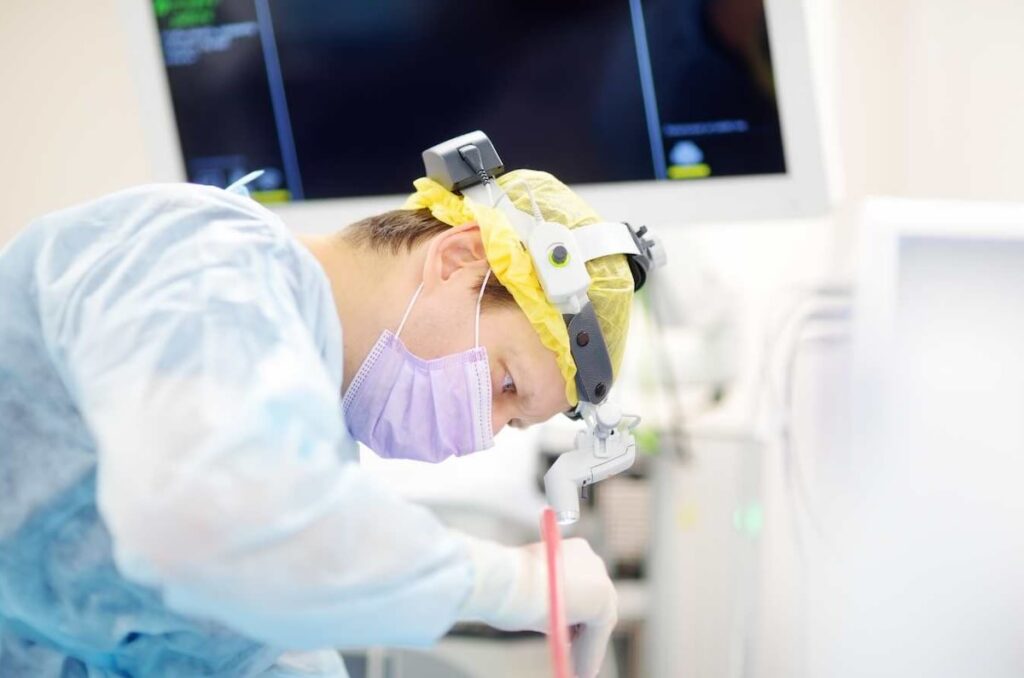
Tissue trauma is injury to the body’s tissue, its building blocks. Such trauma is a possible consequence of surgery and can lead to complications during and after an operation. Surgical teams must proactively avoid tissue trauma during their work by using techniques to protect the tissue.
This article explains why tissue protection matters and gives effective ways to save tissue from injury during surgery.
What is a tissue, and why does it need protection during surgery?
A tissue is a group of cells that work together to perform a particular function. The human body contains four basic tissue types: muscle, nervous, epithelial, and connective.
Muscle tissue moves the body, while nervous tissue controls and coordinates body activities. Epithelial tissue makes up the skin and lines internal organs and body cavities, mediating protection, secretion, and absorption. Connective tissue, as its name suggests, connects and supports other tissues.
Injury to any of these tissues leads to their dysfunction. Dysfunction, in turn, causes complications ranging from pain to organ failure. During surgery, tissues are exposed to mechanical pressure, physical factors, and anesthesia. Injury when once damage thresholds are crossed. Tissues become especially vulnerable when they do not get enough blood or become infected. Old age and advanced sickness also increase the risk of injury.
Various surgery-related causes can damage tissue. Pressure from surgical positioning is one such cause. Handling instruments carelessly is another. Some surgeries, such as orthopedic surgeries, make tissues especially vulnerable as they use more force.
Tissue protection techniques aim to minimize iatrogenic (doctor-induced) injuries. So, what exactly can surgeons and other team members do to protect tissues effectively?
1. Position the patient optimally
An optimal patient position provides good surgical access while keeping the patient’s body as naturally aligned as possible. It preserves soft tissue, including skin, muscles, nerves, and blood vessels.
Patient positioning is regulated by guidelines that vary depending on the type of surgery. For instance, during abdominal surgery, the patient is placed on their back. During shoulder replacement, the patient is placed in a sitting position. For spine surgeries, the patient lies face-down. Positioning guidelines also consider the patient’s age, body size, and overall health.
Following these guidelines prevents pressure-induced injuries of the skin and soft tissue (pressure ulcers). The practice also maintains good airflow and skin perfusion. Pressure-reducing devices, such as silicone foam, foam mattresses, head pads, and cushions, are used for additional patient comfort.
2. Regulate the patient’s core temperature
Anesthetists and nurses in the operating room should pay close attention to optimizing core temperature during surgery. They should measure it continually and strive to keep it at about 37°C, known as normothermia, which is the state in which tissues function best.
General anesthesia is crucial for performing surgeries. Under general anesthesia, blood flow is typically redistributed from the core to the limbs. As a result, the body’s temperature drops below 36°C, and hypothermia develops. Hypothermia is associated with lowered immunity and a higher risk of surgical site infections and bleeding. Thus, tissues suffer, and life-threatening complications follow.
Hypothermia can be prevented using forced air warming. This technique transfers heat directly to the patient’s skin. It involves placing a self-warming blanket or gown on or under the patient throughout the surgery. Forced air warming applies to any surgery under general anesthesia, regardless of duration.
That said, warming the skin during surgery should be done with caution. High skin temperature and moisture have been shown to increase the likelihood of skin and soft tissue injuries.
3. Choose minimally invasive surgery where possible
Minimally invasive surgery is an increasingly common surgical technique. When applicable, it is often preferred to traditional open surgery. The decision between minimally invasive surgery and open surgery depends on the type of surgery, the patient’s informed preference, and the surgeon’s skill level.
Compared to open surgery, minimally invasive surgery is more tissue-friendly. It involves smaller skin incisions than open surgery. Additionally, it is quicker, safer, and associated with a shorter and less painful recovery time. During minimally invasive surgery, surgeons operate using thin, tubular instruments. Thus, skin and internal tissue manipulation and injury are much less pronounced.

Due to these benefits, operations like appendectomy (the surgical removal of the appendix) are largely performed with minimally invasive surgery.
However, minimally invasive surgery does not always replace open surgery. Colorectal cancer removal surgery is a concrete example in which the open surgical approach is the better surgical technique.
4. Inspect and use instruments properly
Every surgical instrument must be inspected and sterilized before use. A defective, worn-out, or non-sterile instrument causes direct tissue damage and infection. Bone-boring and endoscopic instruments should be closely examined, as they often break during operations.
Surgeons must use instruments without excessive force. To instruct them, researchers have suggested setting tool-tissue force limits. Tool-tissue forces vary depending on the type of surgery and tissue. Characteristically, orthopedic surgeries use the most force, while ophthalmologic procedures use the least.
Grasping instruments, forceps, and retractors are used during both open and minimally invasive surgeries. They stabilize tissues and provide an optimal view of the operating field. However, they also place a lot of mechanical stress on organs, muscles, and nerves. They should not be kept in place for long to prevent tissue compression and ischemia.
Moistened sponges can reduce bacterial contamination. Thus, they can be used to protect soft tissue before applying a retractor. Handheld retractors, where suitable, such as in plastic surgery or dental/oral surgery, may be preferred to self-retaining retractors. They lend greater flexibility and more control over the visible area. Of course, though, they do occupy a hand, which means the surgeon may need help from an assistant to hold the device and ensure proper retraction.
5. Use instrument covers and sheaths
Covers and sheaths increase instrument safety. Polytetrafluoroethylene (PTFE) covers provide a concrete example. PTFE (also known as Teflon) is a durable synthetic polymer. PTFE covers can insulate laparoscopic instruments and, thus, protect the abdominal wall and organs from thermal injuries.
Instrument sheaths are also used in neurosurgery. They notably reduce collateral tissue damage during trans-nasal and eye procedures. This tissue includes the nasal epithelial tissue, the tissue lining and surrounding the frontal, maxillary, and sphenoid sinuses, as well as the tissue around the eye socket.
Using instrument covers and sheaths also applies to orthopedic surgeries involving drills. A drill stopper can protect bones, nerves, and blood vessels by controlling drill penetration depth.
6. Count the instruments and equipment
Surgeons sometimes “forget” instruments inside the body. It is estimated that surgical instruments and other equipment are left inside the body in 1,500 surgeries per year in the US. Common examples of retained surgical equipment include swabs, needles, forceps, and catheters. This malpractice causes complications from tissue compression, infection, and bleeding.
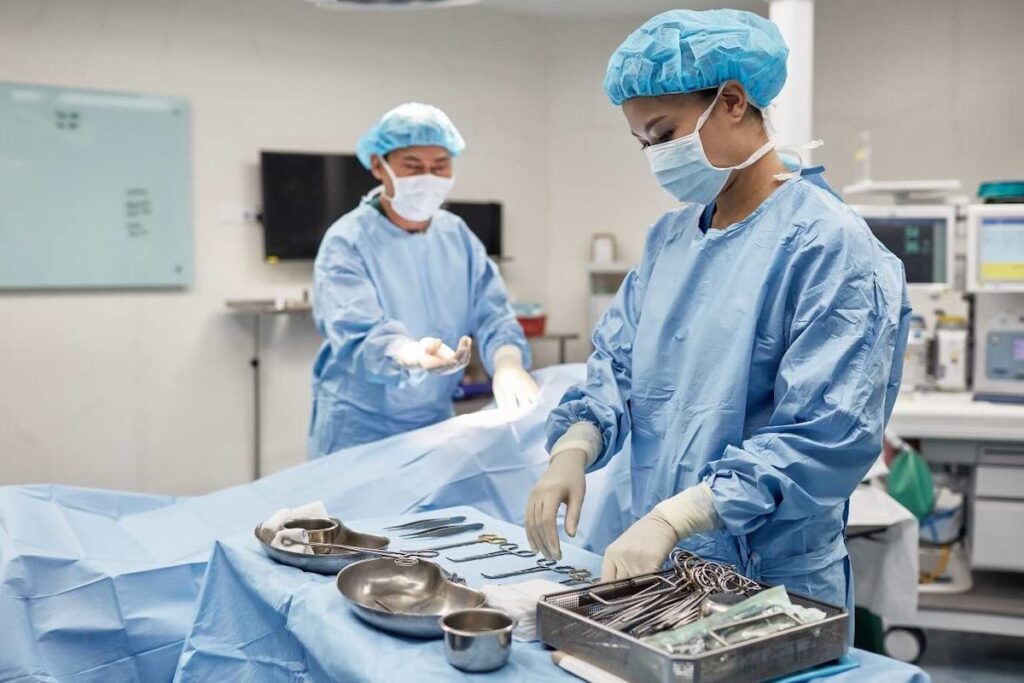
To prevent cases of retained instruments, the IFPN (International Federation of Perioperative Nurses) has devised guidelines (PDF) for adequate surgical counting. According to the guidelines, the operating room nurses must count the surgical equipment before and after surgery is complete. As a rule, these counts must match.
7. Prevent dead spaces and bleeding
A “dead space” is a body cavity left behind after closing an incision. It usually results from removing a tumor, such as a lipoma. Serum or blood collects in dead spaces, compressing or infecting nearby tissue. To protect tissue, surgeons close or eliminate dead spaces with so-called quilting sutures before suturing the skin. In addition, they place a drain that clears out any remaining fluids.
Hemostasis is the action of stopping bleeding. Blood leaks should be recognized and cut off to protect internal tissue and prevent complications. Hemostasis improves the surgeons’ field of view, allowing them to be more precise and save tissue. Surgeons should always double-check for any bleeds before closing off wounds.
8. Reduce operative time
Surgeons should strive to reduce operative time whenever possible. Prolonged surgeries are associated with a higher risk of tissue infection. The risk of surgical site infection increases by 37% for every extra hour of surgery.
Operative time is especially important for long elective surgeries, such as total knee replacement (TKA). TKA procedures lasting longer than 100 minutes significantly increase the risk of deep infection.